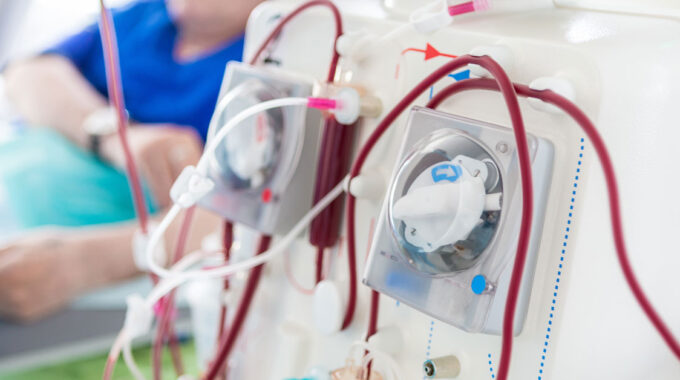
How Will the Vaccine Mandate Affect Hospice Staffing?
Less than two weeks from now, on December 6, the federal government will require COVID-19 vaccination of all hospice employees, volunteers, and subcontractors. Reports suggest this will add to the already growing staffing challenges in hospice, but the White House predicts marginal effects on staffing.
December 6 Emergency Vaccine Mandate for Healthcare
On November 4, 2021, the Centers for Medicare and Medicaid (CMS) published an emergency regulation requiring COVID-19 vaccination for a long list of healthcare providers. The list includes hospice. This mandate does not limit itself to hospice nurses. Everyone who works for hospice must meet the requirement. This includes hospice volunteers, office staff, and subcontractors who deliver care and are paid by the hospice.
Moreover, the emergency regulation covers 76,000 healthcare companies employing 17 million healthcare workers. It requires a first vaccine dose on December 6. For Pfizer and Moderna vaccines, the two-dose regimen needs to be completed by January 4. However, CMS allows for exemptions based on medical conditions or religion. Hospice agencies not in full compliance on December 6 could lose their access to Medicare and Medicaid payments. That would close most hospice agencies.
2021 Hospice Staffing Concerns
In February 2021, Hospice News reported the results of their survey including 161 hospice agencies nationwide. More than a third listed staffing challenges among their top concerns for the year – second only to concerns about access to hospitals during the pandemic. Of course, across all provider types, the nationwide nursing shortage is well documented. What’s more, hospice may feel the pinch more than other providers. The lower Medicare reimbursement in hospice already leads to a trend of lower nurse pay. Payscale finds that hospice nurses make about six percent less than all staff nurses on average.
Do Vaccine Mandates Cause Healthcare Staffing Shortages?
On October 7, the White House refuted reports that COVID-19 vaccine mandates lead to large scale employee turnover. Their report, titled “WHITE HOUSE REPORT: Vaccination Requirements Are Helping Vaccinate More People, Protect Americans from COVID-19, and Strengthen the Economy,” suggests that vaccine mandates cause only marginal changes in healthcare employment. It cites anecdotes in which resignations amount to 1% of staff or less.
On the other hand, other accounts attribute vaccine mandates to staff losses topping 30%. Some states and more than 40 hospitals have already implemented their own COVID-19 vaccine mandates. New York’s statewide vaccine mandate for healthcare workers went into effect September 27. Subsequently, New York’s News 8 WROC reports an overall loss of 3% of healthcare workers in the state. This includes resignations and firings.
On November 4, CMS stated that 29% of healthcare workers remain unvaccinated. That leaves a large potential for staffing challenges in hospice over the next few weeks.
Why Have a COVID-19 Vaccine Mandate in Hospice?
CMS states that unvaccinated staff pose both a direct and indirect threat to the very patients whom they serve, as well as to their co-workers. This rule adds to the historical flu and hepatitis B that states have required. “Ensuring patient safety and protection from COVID-19 has been the focus of our efforts in combatting the pandemic and the constantly evolving challenges we’re seeing,” said CMS Administrator Chiquita Brooks-LaSure. “Today’s action addresses the risk of unvaccinated health care staff to patient safety and provides stability and uniformity across the nation’s health care system to strengthen the health of people and the providers who care for them.”